I could feel my mind going deeper and deeper into a fog. No matter how hard I tried to focus, I couldn’t seem to make sense of the basic problems that I had been tasked with. What is the sum of 15 plus 4? The question wasn’t hard, but it took all of my brainpower to muster up the answer. 19. Next question … I felt generally OK, but there was pressure behind my eyes, I could feel a slight headache coming on and my vision didn’t seem quite right. With the exception of the sheet of paper in front of me, the remainder of the room had faded away. It was time to don the oxygen mask before hypoxia did a number on me.
As soon as the life-critical O2 molecules started to flow back into my arteries I could feel my senses return. It was as if someone had flipped a switch. There were suddenly bright colors on a page that just moments ago had appeared dull; the room opened up as my peripheral vision returned; I could feel my mind start to work again, and that pressure behind my eyes slowly dissipated.
I was at 28,000 feet and in a high-altitude chamber at Edwards Air Force Base — a visit that had been arranged by the San Fernando Valley 99s chapter. The year was 2000 and I was a budding pilot, but the high-altitude training I received was one of the most valuable learning experiences that I’ve had in my flying career. It taught me how to quickly identify symptoms of hypoxia — a state of oxygen depletion in the body that has the potential to swiftly and unnecessarily end a flight in tragedy.
While it is hard to determine whether an accident is caused by hypoxia, investigators do attribute a few accidents to this condition every year. A query in the National Transportation Safety Board’s aviation accident database found 24 accidents related to hypoxia in the past decade. Twenty-two of them included fatalities.
2014 presented two tragic accidents within about a week’s time that may have been caused by hypoxia. An NTSB report tells the story of how, on Aug. 30, a Cirrus SR22 pilot flying at 21,000 feet became unresponsive to ATC, flew right through a restricted area near Washington, D.C., and eventually crashed into the Atlantic Ocean, 35 miles east of Wallops Island, Virginia. Pilots flying the airplanes that intercepted the Cirrus reported that the pilot appeared to be unconscious.
Just one week later, on Sept. 6, a TBM 900 pilot reported a problem in the cockpit to air traffic control and requested a descent from 28,000 to 18,000 feet. ATC cleared him to 25,000 feet, to which he replied: “We need to get lower.” Soon after, the pilot became unresponsive and the airplane later crashed near Jamaica.
Recognizing oxygen depletion early could save your life, but hypoxia is very difficult to detect since its symptoms vary significantly from person to person. There is really no altitude at which you can be completely safe from hypoxia. But with the right equipment in the cockpit, you can help prevent this debilitating state.
WHAT IS HYPOXIA?
Hypoxia is a deficiency of oxygen, and without enough of it your body cannot function properly. The body absorbs oxygen through each breath of air, which consists of 78 percent nitrogen, 21 percent oxygen and 1 percent of various other gases. These percentages remain relatively constant as you climb higher and higher into the atmosphere. At greater elevation the air is less dense, which decreases the body’s ability to absorb oxygen.
While the air density is affected by elevation, temperature and pressure, the amount of oxygen at altitude is somewhat predictable. Robert Jamieson, CEO of Redmond, Oregon-based Mountain High Equipment and Supply Co., says the atmospheric pressure at 10,000 feet is approximately two-thirds of that on the ground, so there is only two-thirds as much oxygen available to breathe.
Just like a fire needs oxygen to burn, the body needs it to function. As you take a breath of air the oxygen flows into the lungs, where the membranes that make up tiny sacs called alveoli transfer the molecules into the bloodstream. Once there, the oxygen is transported by hemoglobin, which carries the molecules in the stream of life to various cells around the body like miniature ships bringing lifesaving supplies to the needy. The cells use the oxygen in a process called cellular respiration, in which nutrients and oxygen are processed into adenosine triphosphate, or ATP, considered by biologists to be the currency of life.
There are several ways for the body to become hypoxic in the cockpit, and there are different terms for each. The most common type of hypoxia is hypoxic hypoxia, which you would experience at an altitude where the air density, or partial pressure, is insufficient to supply enough oxygen in each breath. You can also experience hypoxic hypoxia by blocking the airways to the lungs by holding your breath or by other means, but there is no good reason to do that in flight.
Another form of hypoxia that pilots experience is called hypemic hypoxia. It happens when the hemoglobin molecules are unable to transport the oxygen that you inhale. Unlike oxygen, carbon monoxide molecules bind irreversibly to hemoglobin, so if your body is breathing CO the little ships become fully loaded and can no longer transport the O2 to the needy cells even if the gas is present in your lungs.
There are other molecules that can mess with the cells’ ability to use oxygen — a condition called histotoxic hypoxia. Alcohol, tobacco and other drug use can cause histotoxic hypoxia, making you experience hypoxic symptoms at a much lower altitude.
Finally, stagnant hypoxia, which happens when blood flow is restricted — a condition that you have likely experienced after crossing your legs too long — can be experienced by pilots during high-G maneuvers, such as when positive G-forces move the blood away from the brain, causing a temporary blackout. While this condition doesn’t last long, aerobatic pilots should be aware.
However hypoxia is achieved, what makes it a particularly dangerous condition is that each one of us becomes hypoxic at different altitudes and different G-forces depending on the amount of regular exposure to those conditions. Also, the symptoms of hypoxia are hard to identify and vary from person to person.
WHAT ARE THE SYMPTOMS?
Hypoxia presents symptoms such as euphoria, decreased reaction time, headache, and impaired judgment and vision, just to name a few. You can also get tingling sensations in the fingers and toes, and cyanosis — in which the fingernails and lips turn a slight shade of blue. These symptoms are difficult to identify whether you have experienced them before or not. The only way to really know how your body will react to hypoxic hypoxia is by exposure in a safe environment like a high-altitude chamber or by flying at a high altitude with another pilot who is breathing supplemental oxygen.
My first identifiable symptom is slight pressure behind my eyeballs. What follows is a fuzzy feeling in my brain and a headache. I’ve also felt a swelling sensation in my fingertips and experienced a limited field of vision. Since the inability to think clearly is hard to identify unless you’re in a controlled environment, it is nearly impossible to determine when that symptom sets in. But I definitely experienced this subtle and highly disconcerting symptom in the altitude chamber.
Whether you can identify your symptoms or not, they will intensify and grow in number as the altitude and time of exposure increase. Eventually the body will shut down. At what point your body becomes incapacitated depends on your ability to tolerate the high-altitude environment. Tibetans surprisingly have a lower count of hemoglobin than other people, and their bodies have genetically adapted to the high-altitude environment. But generally the most noticeable acclimatization to higher altitudes is an increase in the production of hemoglobin molecules, allowing the body to transport any available oxygen more efficiently.
With extreme acclimatization, people such as the amazing Italian mountaineer Reinhold Messner have climbed to the top of Mount Everest, which tops out just above 29,000 feet, without supplemental oxygen. That means that Messner spent hours above what mountain climbers refer to as the death zone, which is defined as any altitude above 8,000 meters — just above 26,000 feet.
Most people would pass out long before reaching such extreme altitudes, even for a few minutes. According to data published by the FAA, the average time of useful consciousness at 30,000 feet is one to two minutes. So if you are flying at altitudes like these, it is critical to always be prepared for a loss of pressurization or an issue with the oxygen supply. Even at 22,000 feet you will likely pass out within 10 minutes if you don’t breathe supplemental oxygen or descend rapidly to a lower altitude.
A person with poor circulation or restricted arterial flow will suffer from hypoxia at lower altitudes and is also more prone to serious conditions such as a stroke or heart attack, says Dr. Brent Blue, a physician who has served as an aviation medical examiner for over 30 years and founded Aeromedix.com, which offers safety, medical and survival equipment for pilots.
WHEN SHOULD YOU USE OXYGEN?
The practical test standards to achieve a private pilot certificate include knowledge requirements for hypoxia, and many examiners will ask about the rules for supplemental oxygen use during the oral exam. As you probably already know, 14 CFR 91.211 requires pilots to breathe supplemental oxygen any time the cabin pressure exceeds 14,000 feet or 12,500 feet for more than 30 minutes.
What you may not be aware of, however, is how those numbers were achieved. Blue says the numbers were not based on human physical requirements but rather on geographical constraints. As a result, as long as you stay within the borders of the lower 48 states, you can fly across the country without legally being required to bring supplemental oxygen.
This raises the question: Are you safe at 12,000 feet? There is a possibility that the answer to that question is a resounding yes. Again, it depends on your body’s ability to tolerate the lower partial pressure of oxygen. If you live in Aspen, Colorado, which is situated in the Rocky Mountain range at nearly 8,000 feet, you may feel great at 12,000 feet for hours on end. However, if you are a relatively healthy sea-level dweller like myself, you will likely need oxygen somewhere between 8,000 and 10,000 feet. Blue says there are some people, particularly those with poor circulation, who need supplemental oxygen at as low as 6,000 feet. The FAA recommends oxygen use above 5,000 feet at night, because the eyes require even more oxygen for night vision.
The only way to truly know whether your body is getting enough O2 is by monitoring your blood through a pulse oximeter. The sidebar talks more about the use of a pulse oximeter and other oxygen equipment.
While the danger of incapacitation is of greatest concern, mild hypoxia will both impair your ability to fly at your peak performance level and leave you drowsy for hours after your flight. So having that extra boost of oxygen will make you more alert during both the flight and the remainder of the day. There is a reason why there are oxygen bars in Las Vegas.
If you are fortunate enough to fly a pressurized airplane, you don’t need to breathe oxygen since the system brings the cabin altitude down. But make sure you have a backup oxygen system ready if you plan to fly above 18,000 feet, as hypoxia will quickly set in if the pressurization system fails.
If you don’t feel the need to use oxygen on the flight, it will come in handy as you get closer to your destination. Blue recommends that you start breathing oxygen about 15 minutes before the estimated arrival. This oxygen boost will energize you and make you more likely to perform at your best when it comes to the most complex part of your flight — the landing.
**
OXYGEN EQUIPMENT**
There are several oxygen systems and monitors that, if used properly, will just about eliminate your risk for developing hypoxia. Whether you use supplemental oxygen to make sure that you have enough at all times or a piece of equipment that ensures your blood is saturated enough with the life-critical gas, you can prevent this debilitating condition. Here are some of the most vital pieces of equipment that you may want to consider if you don’t already have them in the cockpit.
Built-in oxygen: Aside from pressurization, a built-in oxygen system is the most convenient way to get your O2. Several companies offer systems that can be installed under a field approval or supplemental type certificate (STC). The only drawback of built-in systems is cost — a few thousand dollars.
Portable oxygen: There are many options for portable oxygen systems, from solo systems that start as low as $200 to systems for multiple users that cost more than $1,000. You can save money by using cannulae that restrict the flow of oxygen during exhalation and that have individual flow meters.
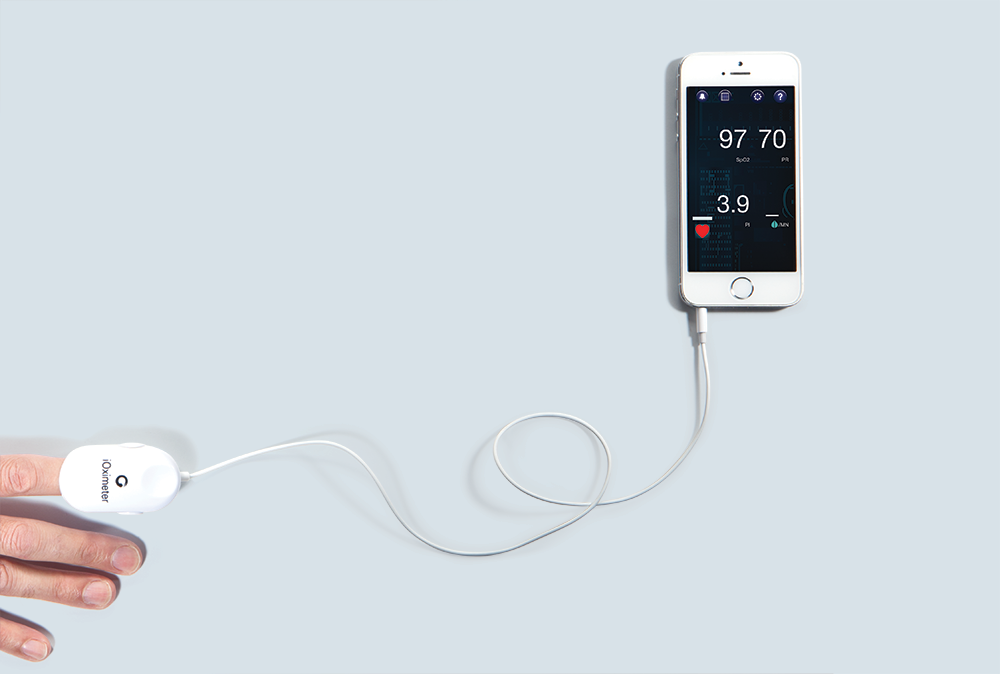
Pulse oximeter: A pulse oximeter measures the oxygen saturation in the blood through a small device that clips onto your finger. Your goal is to adjust the oxygen flow to maintain the displayed number within 5 percent of the normal saturation, which is generally 98 percent. Starting at around $50, a pulse oximeter is a great investment.
Carbon monoxide detector: The only way that a pulse oximeter can trick you is if carbon monoxide enters the body. A very basic carbon monoxide detector costs just a few dollars, while digital detectors will cost $100 and up.
Oxygen concentrators: Frequent oxygen users may want to consider an oxygen concentrator, which generates oxygen. The cost starts at around $2,000.
Pulse-demand system: Mountain High’s patented Electronic Delivery System (EDS) predicts when your body is ready to inhale. At that precise moment, the system delivers a shot of O2, greatly limiting the use of oxygen. A one-person EDS-O2D1 kit, which includes two cannulae and a face mask, costs $650.
Get online content like this delivered straight to your inbox by signing up for our free enewsletter.






